Tekst: Dr Dean H Watson Director, Watson Headache Clinic; Director, Watson Headache Institute Clinical Consultant in Headache and Migraine International Headache and Migraine Educationalist
As a trained physiotherapist the chances are you were taught that the only form of headache you can treat is cerviocogenic headache. You may be surprised to hear that within the traditional medical model of headache, debate continues as to whether cervicogenic headache exists! It doesn’t get much better when, those advocating for the existence of cervicogenic headache, estimate its prevalence to be around only 4 per cent!
The diagnostic criteria are more challenging for cervicogenic headache than those for primary headache i.e. migraine and tension headache; if the criteria are strictly applied, then it is not surprising that cervicogenic headache is a rarely diagnosed. This situation does a disservice to headache and migraine sufferers; why is that that those who established the diagnostic criteria for cervicogenic headache – a musculoskeletal condition – are not experienced in musculoskeletal medicine?
According to the traditional medical model, cervcogenic headache is unilateral and side locked i.e. it always occurs on the same side. Yes, often it is. This means though that a unilateral headache that can occur on either side, either between episodes of within the same episode is not cervicogenic headache – absolute nonsense. An alternating headache is the C2-3 equivalent of an alternating lumbar list (contralateral to lumbar pain). A palpation examination reveals rotation of C2 contralateral to the side of (predominant / most frequent) headache, i.e., the spinous process will be deviated towards the side of pain.
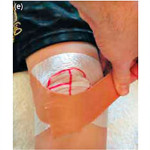
As manual / physio therapists, we rely on temporary reproduction of accustomed head pain when examining upper cervical structures; indeed this is one of the key diagnostic criteria of cervicogenic headache. I disagree – there are situations when you will be able to reproduce familiar head pain and it not be cervicogenic headache. What is more definitive is resolution of the referred head pain as the examination technique is sustained.
Now for a paradigm shift… the term ‘cervicogenic headache’ does a disservice to the role of cervical afferents in primary headache. I wish we could move away from using the term ‘cervicogenic headache’ – it polarises the medical headache world.
Let’s consider some facts:
- the underlying disorder in migraine and tension headache is a sensitised brainstem i.e. migraine and tension headache are not separate disorders, they are different manifestations of the same disorder1,2
- the triptans (specific anti migraine medication) abort migraine,2,3 tension headache,2,3 cluster headache,4-7 menstrual migraine8-11 (yes – menstrual migraine is not about hormones – do hormones affect one side of the head only?), and cervicogenic headache,12 by desensitising the brainstem
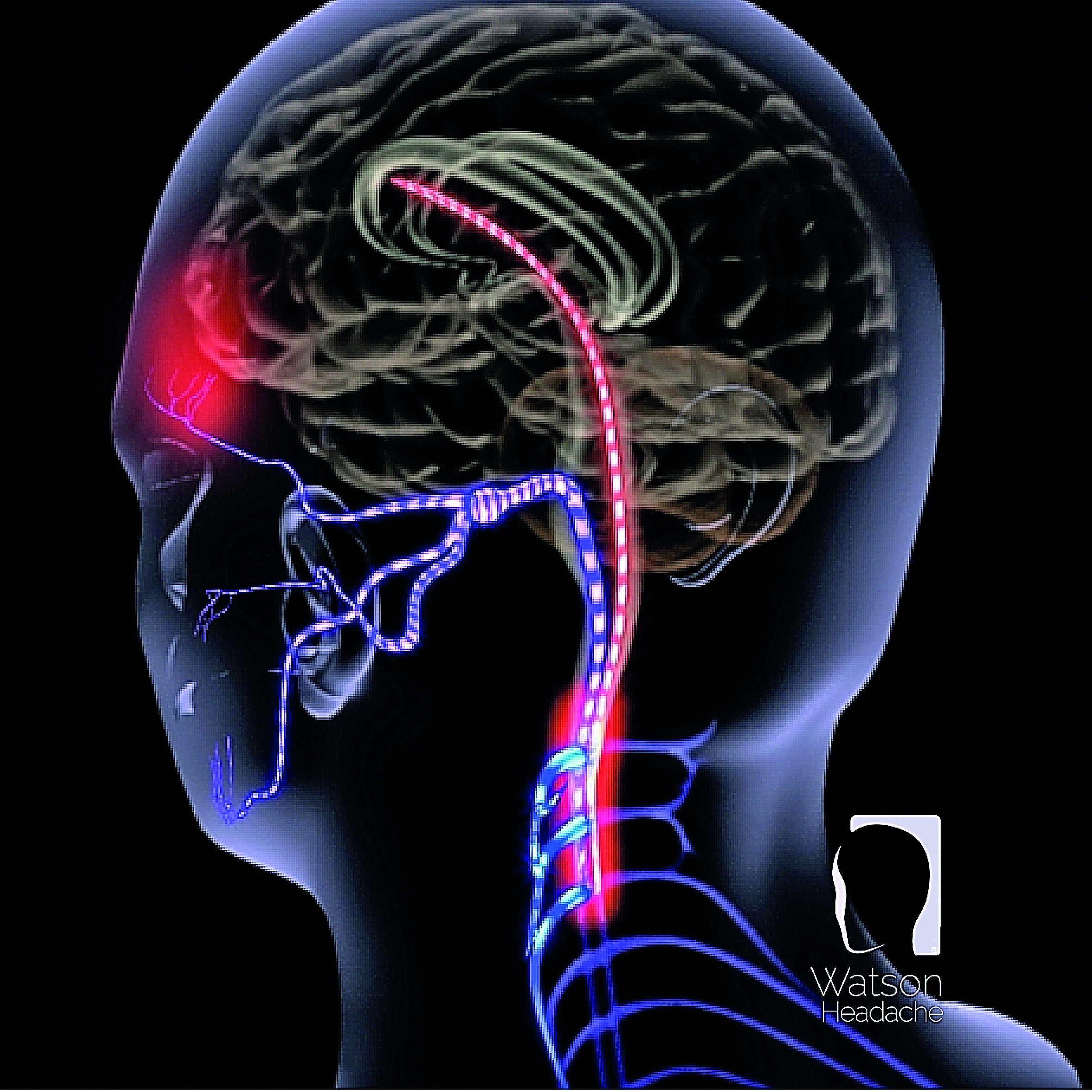
- the C1-3 spinal afferents converge on the brainstem13,14 i.e., noxious afferent information has the potential to sensitise the brainstem15
- manual cervical reproduction and resolution of accustomed head pain in migraineurs desensitises the brainstem16
- 80 per cent of migraine alternates i.e. swaps sides.17,18 Supposedly this feature differentiates migraine from cervicogenic headache. Yes it does, but not in the way the medical model would have it. Alternating headache or headache with side shift is the one subjective feature that confirms cervicogenic headache.
Diagnosing primary headache relies on signs and symptoms it doesn’t tell us what the cause is. Surely optimal management is about determining the reason for sensitisation of the brainstem and elementary neuro anatomy shows us that noxious C1-3 cervical afferents are ideally placed to sensitise
the brainstem.15 Furthermore unequivocal confirmation of the relevancy of noxious C1-3 afferents in a headache condition is straightforward.16
References available at http://www.watsonheadache.com/more-than-just-a-headache